A mouse model for Dry Eye Disease

Experimentica utilizes a validated mouse model of dry eye disease. Dry eye disease-like pathology is induced using transdermal scopolamine patches in combination with desiccating environmental stress. The induced pathology is characterized using corneal fluorescein staining, tear volume measurements, and histology for lacrimal gland infiltration, goblet cell loss, and corneal abnormalities.
Dry eye disease, also referred to as keratoconjunctivitis sicca, dry eye syndrome, and dysfunctional tear syndrome, is a multifactorial ocular surface disease characterized by ocular discomfort, irritation, and visual disturbance. It ranks among the most frequently encountered ocular morbidities, with more than 25% of patients attending ophthalmic clinics reporting these symptoms (Dana et al. 2019).
The global prevalence of dry eye disease is estimated to range from 7% to 34%, depending on diagnostic criteria and the population surveyed (Deo and Nagrale 2024). The steep rise in annual dry eye disease incidence and prevalence over the past decade has recently been estimated (Zhang et al. 2024).
In 2002, Dursun and colleagues published a mouse model of dry eye disease by combining application of transdermal scopolamine patches together with a desiccating environmental stress (Dursun et al. 2002). At Experimentica, we use corneal fluorescein staining (CFS) to confirm successful model induction.
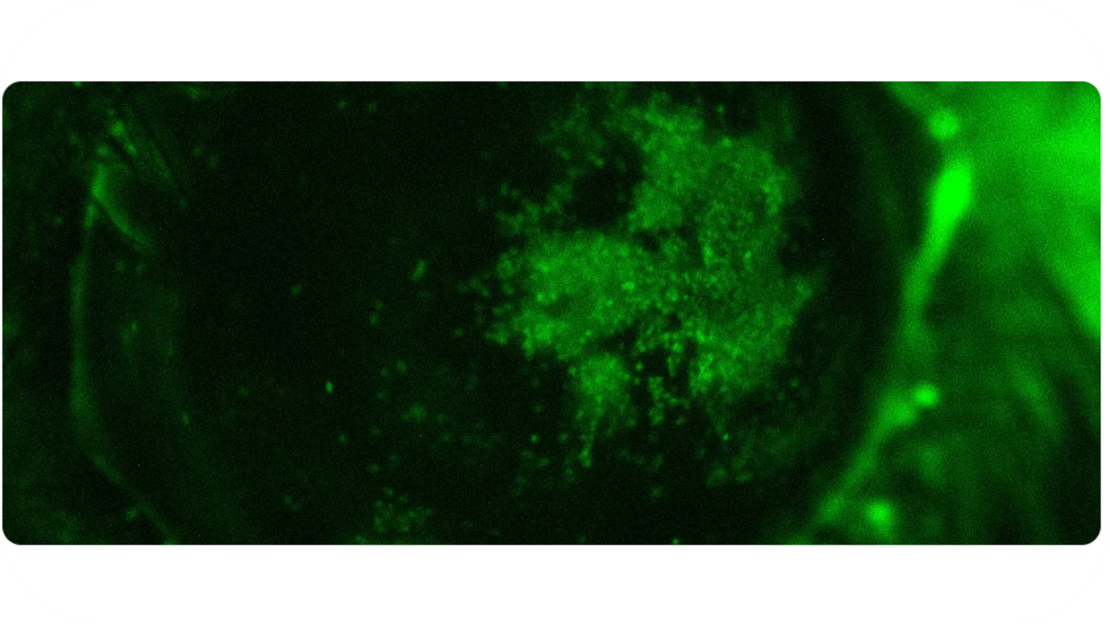
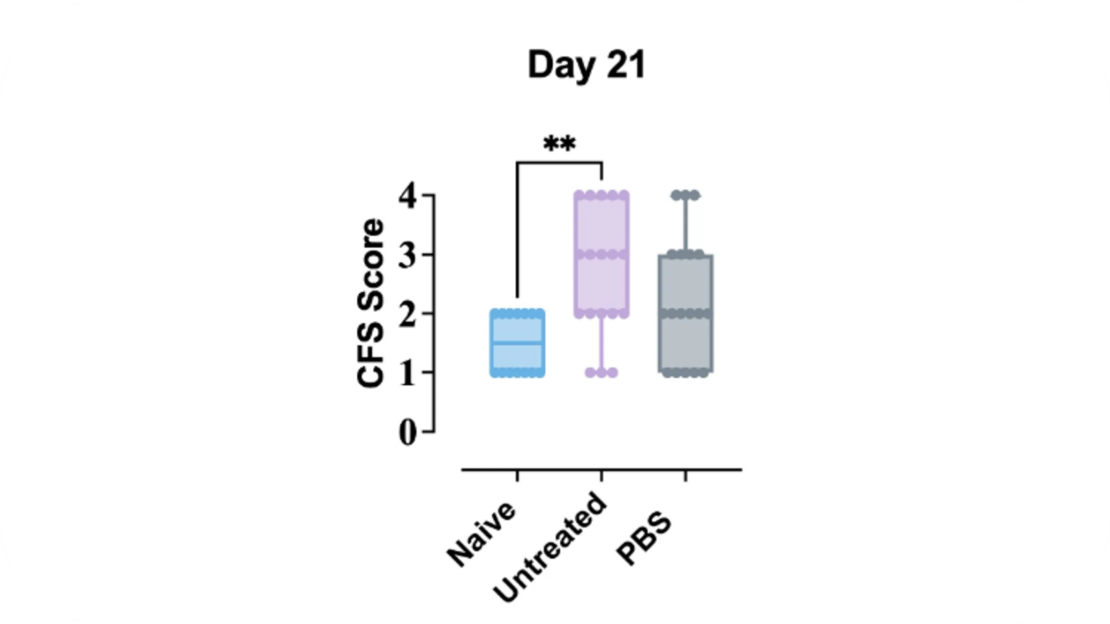
CFS is scored using the modified Oxford score method by assigning scores from 0 (healthy corneal epithelial cell layer with no observable fluorescein staining) to 4 (severe corneal epithelial cell damage with widespread confluent staining of the cornea.
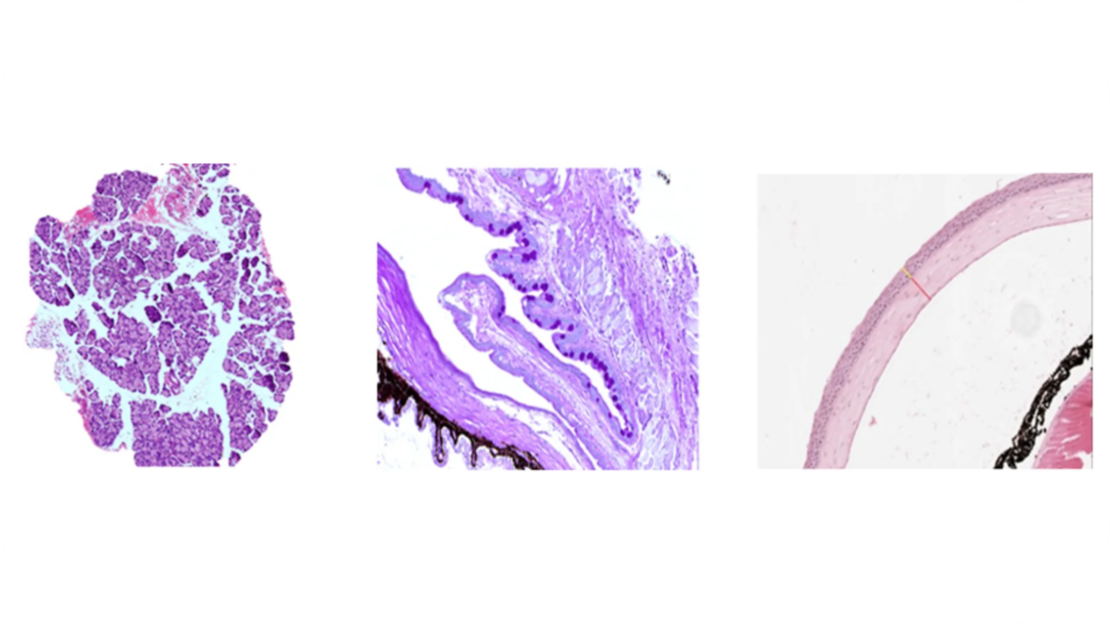
In addition, the evaluation of dry eye disease-like pathology can be performed with tear volume measurements and histological assessment of immune cell infiltration in lacrimal glands, quantification of goblet cells in the conjunctiva or corneal thickness and the number of corneal epithelial layers.
Contact us for more information or schedule the meeting with our experts!
Contact usLearn more about our Dry Eye Disease model
References
-
- Dana, Reza, John L. Bradley, Annie Guerin, Irina Pivneva, Ipek Özer Stillman, Amber M. Evans, and Debra A. Schaumberg. 2019. “Estimated Prevalence and Incidence of Dry Eye Disease Based on Coding Analysis of a Large, All-Age United States Health Care System.” American Journal of Ophthalmology 202:47–54. doi:10.1016/j.ajo.2019.01.026.
- Deo, Niyati, and Prachee Nagrale. 2024. “Dry Eye Disease: An Overview of Its Risk Factors, Diagnosis, and Prevalence by Age, Sex, and Race.” Cureus 16(2):e54028. doi:10.7759/cureus.54028.
- Zhang, Han, Kuiliang Yang, Wanju Yang, Shanshan Wan, Yanning Yang, and Yiqiao Xing. 2024. “Epidemiological Characteristics of Dry Eye Disease in Asian and Asian Female Populations: A Database-Driven Descriptive Study.” Journal of Current Ophthalmology 36(2):159–67. doi:10.4103/joco.joco_46_24.
- Dursun, Dilek, Min Wang, Dagoberto Monroy, De-Quan Li, Balakrishna L. Lokeshwar, Michael E. Stern, and Stephen C. Pflugfelder. 2002. “A Mouse Model of Keratoconjunctivitis Sicca.” Investigative Ophthalmology & Visual Science 43(3):632–38.



